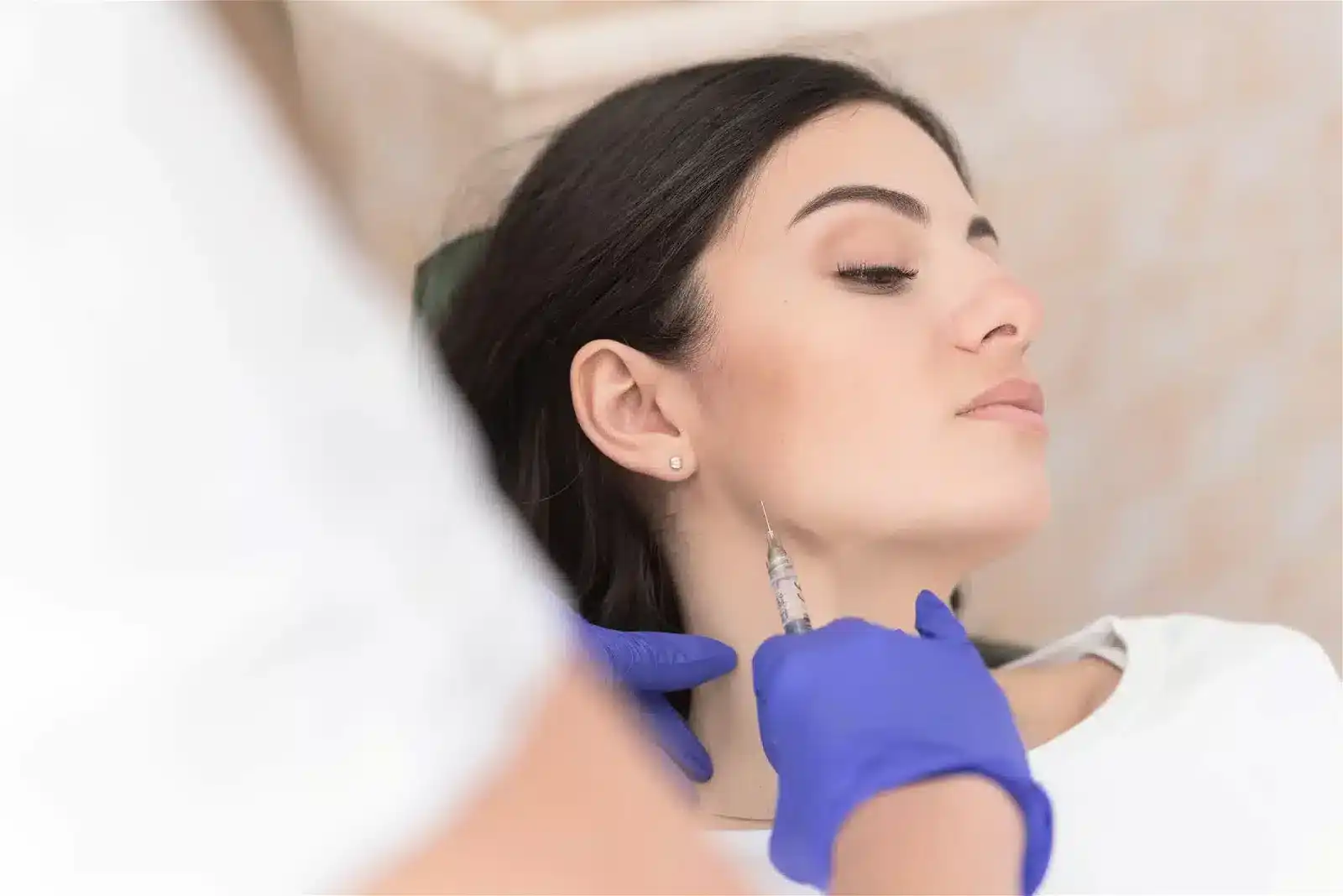
Botox for TMJ
David Fuller
Last Updated On: October 15, 2024
Innovative treatment approaches are continuously emerging to address various medical conditions. Temporomandibular Joint Disorder (TMJ), a complex condition causing jaw pain and discomfort, is no exception.
In recent years, medical professionals have explored Botox as a potential treatment for TMJ, and the results are very interesting. This article aims to answer the question – “Does Botox help TMJ dysfunctions?”
What is TMJ?
Temporomandibular Joint Disorder, commonly known as TMJ or TMD, refers to the conditions affecting the temporomandibular joint, connecting the jawbone to the skull. This joint is crucial in everyday activities like speaking, chewing, and swallowing.
TMJ disorders can manifest as a range of symptoms, including:
- Jaw pain and tenderness;
- Clicking or popping sounds during the jaw movement;
- Locking of the jaw;
- Difficulty in opening or closing the mouth;
- Headaches and facial pain.
These symptoms can significantly impact a patient’s quality of life, leading them to seek effective treatment options.
How Does Botox Help TMJ?
Like other botulinum toxins, Botox blocks nerve signals in the muscles where it is injected, leading to muscle relaxation. This effect is widely used in medicine and for aesthetic purposes.
Botox is considered beneficial in the context of a TMJ treatment due to its muscle-relaxing properties. The temporomandibular joint is surrounded by a complex network of muscles responsible for jaw movement. In cases of TMJ disorder, these muscles may become tense, leading to pain and dysfunction. Botox can alleviate this tension by temporarily weakening the affected muscles.
It is essential to remember that receiving Botox treatment for another medical condition or using it in cosmetic applications won’t be effective against TMJ. You’ll need a specific TMJ-targeting procedure and precise needle injection technique to get adequate results.
Here’s how Botox helps for TMJ:
- Botox injections directly target the overactive jaw muscles responsible for TMJ symptoms. Botox can ease jaw tension, reduce pain, and improve jaw mobility by reducing muscle activity.
- TMJ patients often experience chronic pain and discomfort. Botox’s muscle-relaxing effect can provide relief from these symptoms, offering patients a better quality of life.
- Many individuals with TMJ also suffer from bruxism, the habit of grinding or clenching teeth. Botox can reduce bruxism by relaxing the jaw muscles involved in teeth grinding, mitigating tooth damage and pain.
- Botox treatments for TMJ dysfunction are minimally invasive compared to surgical options, making them an attractive choice for patients seeking relief without extensive procedures.
Benefits & Risks of Treating TMJ with Botox
As with any medical treatment, Botox therapy for TMJ comes with its own set of benefits and potential risks that doctors should carefully consider before recommending it to patients.
Benefits:
- A non-surgical option for TMJ treatment.
- Provides pain relief for patients suffering from TMJ-related discomfort, headaches, and sometimes even migraines.
- Improves jaw function by relaxing overactive muscles, reducing jaw locking, and limited mouth opening symptoms.
- Botox can help manage bruxism, preventing further damage to teeth and related oral structures.
- Quick procedure, requiring minimal downtime for patients.
Risks:
- Common adverse effects of Botox injections include redness, bruising, swelling, and sometimes temporary weakness in nearby muscles. Also, nausea, muscle pain, dry mouth, headache, flu-like symptoms, eyelid droop, and facial muscle paralysis might occur after the treatment. These effects are generally mild and do not last long.
- Long-term studies on the safety and effectiveness of Botox injections for TMJ are limited, which may pose some uncertainty about its sustained benefits and risks.
- Botox treatments may be costly, especially when multiple sessions are required for long-term symptom management.
- Botox use for TMJ is not FDA-approved yet.
- Not all TMJ patients are suitable candidates for Botox treatment. Doctors must carefully evaluate each patient’s condition and medical history before recommending Botox.
TMJ Treatment Procedure With Botox
Doctors must have a thorough understanding of the anatomy of the jaw, the specific muscles involved in TMJ, and proper injection techniques to ensure the safe and effective administration of Botox.
The procedure for treating TMJ with Botox involves several steps:
- A comprehensive evaluation of the patient’s TMJ condition on a preliminary consultation helps determine the suitability of Botox treatment.
- Doctors should thoroughly explain the procedure, potential risks, benefits, and expected outcomes to the patient.
- They will then identify the muscles responsible for TMJ symptoms and select the appropriate injection sites.
- Before drug administration, a numbing cream or an icepack might be used to minimize the pain and discomfort during the procedure. After that, Botox is injected into the targeted muscles with a fine needle. The number of injections and the amount of Botox used depend on the severity of the patient’s condition and their individual factors.
- After the treatment, patients must sit upright for several hours to prevent the botulinum toxin from moving into other areas around the injection zone. They are also advised to avoid strenuous activities and massaging the treated area immediately after the procedure. Ice packs or applying cold compresses may be recommended to reduce swelling.
Patients may require multiple sessions over time, as Botox’s effects are temporary. Doctors should schedule follow-up appointments to assess the treatment’s effectiveness and determine if additional injections are needed. Continuous monitoring of the patient’s progress is essential to adjust treatment plans as necessary.
Alternative Treatments for TMJ
While Botox has gained some attention as a promising treatment for TMJ, it’s important to consider alternative therapies and approaches, as not all patients may benefit from or be suitable candidates for Botox. Some alternative treatments and interventions for TMJ include:
- Oral appliances, such as custom-made oral splints or mouthguards, can help align the jaw correctly and reduce TMJ symptoms by preventing teeth grinding and jaw clenching.
- Jaw exercises and manual therapies can improve jaw mobility and reduce muscle tension.
- Non-steroidal anti-inflammatory drugs (NSAIDs) and muscle relaxants may temporarily relieve TMJ symptoms.
- Stress often exacerbates the condition, so its management using stress reduction techniques like relaxation exercises or counseling can help manage TMJ symptoms.
- In cases where misaligned teeth contribute to TMJ, orthodontic treatments like braces or Invisalign may be recommended.
- In severe cases of TMJ where patients do not respond to conservative treatments, surgical options such as arthrocentesis, arthroscopy, or open joint surgery should be considered.
Conclusion
Using Botox as a treatment for TMJ represents a growing trend in the medical field, offering potential benefits in pain management, muscle relaxation, and improved jaw function. However, doctors must consider their patient’s needs and preferences and carefully evaluate the risks and benefits before recommending Botox therapy.
As research on Botox for TMJ continues, healthcare professionals must stay informed on the latest developments and evidence to provide the best possible care for their patients experiencing TMJ-related symptoms.
FAQ
How long does Botox last on TMJ?
In TMJ treatment, Botox’s effects can vary from person to person but typically last between 3 to 4 months. As the Botox begins to wear off, TMJ-related symptoms, such as jaw pain, muscle tension, and headaches, may gradually return.
To maintain the benefits of Botox for TMJ, patients usually require repeat injections at regular intervals. Most dentists recommend scheduling follow-up injections before the previous dose wears off to ensure continuous relief.
Does Botox help with TMJ?
Botox has shown promise as a treatment for temporomandibular joint disorder (TMJ), particularly for managing specific symptoms – relaxing tense jaw muscles and alleviating pain.
However, Botox does not address the root causes of TMJ, such as:
- joint misalignment;
- structural issues;
- underlying medical conditions.
The effects of Botox treatment are temporary, typically lasting for several months, meaning that repeat injections are necessary to maintain symptom relief.
How many Botox sessions are required for TMJ?
The amount of Botox sessions required for TMJ treatment varies from patient to patient, based on the individual treatment response and the severity of their condition. Generally, patients have required one or two Botox applications before it is possible to assess the effectiveness. If the treatment does prove beneficial, they may proceed with periodic sessions, typically at an interval of three to four months, in order to maintain symptom relief.
Regular follow-up evaluations will help determine if additional sessions are necessary for managing TMJ symptoms effectively.
References
Cao PT. The use of botulinum toxin and dermal fillers to enhance patients’ perceived attractiveness. Dental Clinics of North America. 2020;64(4):659-668. doi:10.1016/j.cden.2020.06.003.
Sonone TP, Soni V, Gupta SD, Shekatkar Y, Thorat AS, Pol T. Botox and dermal fillers in orthodontics – A review. Journal of Pharmacy and Bioallied Sciences. 2022;14(5):60. doi:10.4103/jpbs.jpbs_184_22.
Blanco-Rueda JA, López-Valverde A, Márquez-Vera A, Méndez-Sánchez R, López-García E, López-Valverde N. Preliminary findings of the efficacy of botulinum toxin in temporomandibular disorders: uncontrolled pilot study. Life. 2023;13(2):345. doi:10.3390/life13020345.
Products
Cart
Log In
Newsletter
Subscribe for exclusive offers and updates on new arrivals
Share feedback at:
Working Hours
MON - SUN 9AM to 6PM EST
The Most Popular Brands
Med Supply Solutions
Support
Secure checkout is guaranteed with full adherence to PCI DSS payment standards.
Products listed here are guaranteed authentic and manufacturer-sourced.
Copyright 2025. Med Supply Solutions
Pay easily with trusted providers

